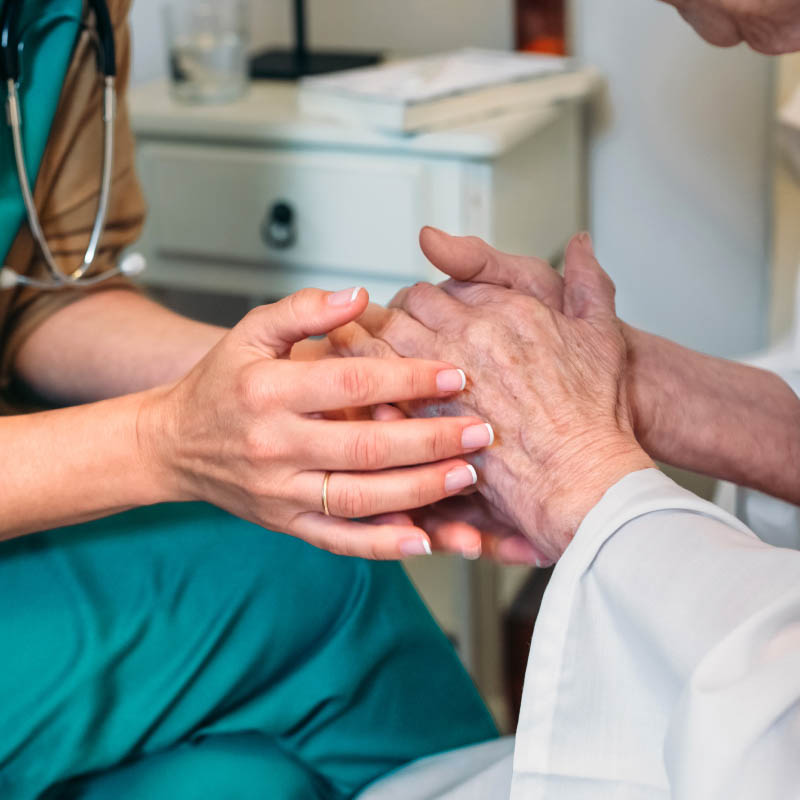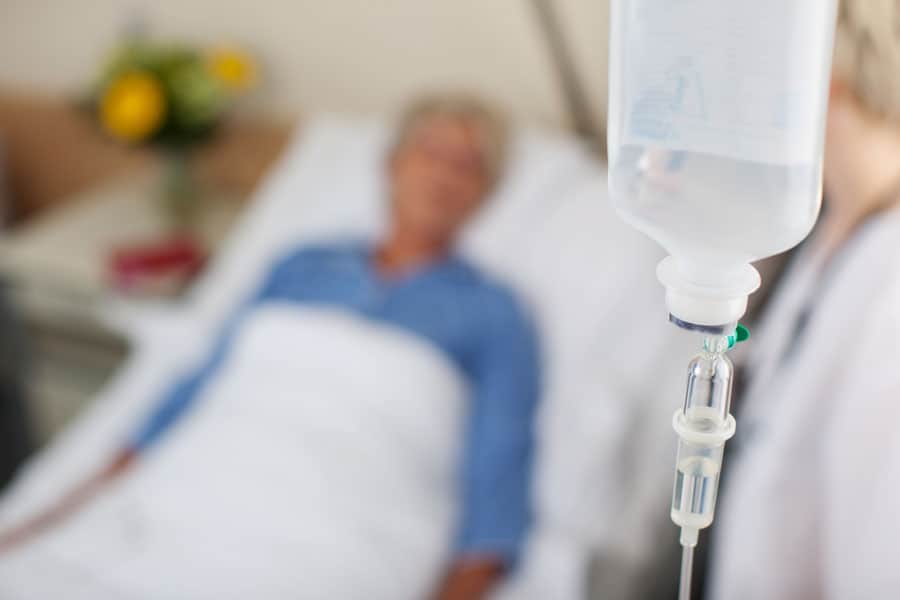
Should a Hospice Patient Receive IV Fluid and a Feeding Tube?
One of the most common questions encountered by Connecticut Hospice staff from concerned family members of patients is whether their loved one will be provided with IV fluids if they cannot eat or drink, or if they should have had a feeding tube placed. The family members of patients with feeding tubes are often uncertain about whether formula feeds should be continued.
Quality of Life and Patient Condition
These are excellent concerns – and understandable. If a patient is no longer able to eat solid foods or drink fluids, it would seem logical that IV fluids would benefit them, that a feeding tube might be in order, or that a preexisting feeding tube should remain in use. The answers to these concerns depend on two more questions. One, why are they no longer able to take food or fluids by mouth? Two, if they are no longer able to eat or drink, what is their quality of life?
Dysphagia and the Risks of Aspiration
Many hospital patients are told that they are at risk of inhaling particles of food and fluid while eating and drinking. This kind of difficulty with swallowing is called dysphagia, a lack of coordination of the muscles that allow us to swallow, and it is very common, especially in elders and even more so in elders with dementia. Inhaling food or fluid, called aspiration, can lead to serious problems, including choking and a form of pneumonia called aspiration pneumonia. A test called FEES, fiberoptic evaluation of swallowing, is used to assess swallowing. In this procedure, a thin endoscopy catheter is threaded into the nose and down to the back of the throat, or pharynx, where the and epiglottis, the little thumb like projection at the top of the windpipe, or trachea, can be observed directly. Once in place, the patient is asked to swallow a bolus of food or fluid. Normally, the epiglottis closes and covers the entrance to the trachea when we swallow. If closure is incomplete, or mistimed, food and fluid can get into the windpipe – aspiration — and cause the problems described above. When this is observed during a FEES test, doctors describe the patient as having “failed” the swallow evaluation – an unfortunate turn of phrase. Even, worse, when dysphagia and the risk of aspiration is diagnosed, patients may be told they cannot eat for fear of the complications. In the interim, they may have a tube inserted into their nose and pushed into their stomach, an NG tube, to be used for feeding, or even undergo placement of a feeding tube directly through the wall of the abdomen into the stomach.

Candidates for IV Eating and Drinking
For some, this is fine. The victim of a stroke, for example, may have a very high risk of serious aspiration with its related complications, as well as significant neurologic impairment such as one-sided paralysis, but still have a good quality of life, and would be an excellent candidate for a feeding tube to provide the nutrition and water necessary to stay alive. I have known people with stroke who were fed by feeding tube continue to enjoy life for years. An elder with advanced dementia, on the other hand, with a very poor quality of life – bedbound, little conscious understanding or enjoyment of life – would not be a good candidate, at least from the medical perspective. In fact, counterintuitive as it seems, feeding tubes, or “PEGS” (percutaneous endoscopic gastrostomy tubes) have been shown to cause more harm than good in elders with advanced dementia, leading to bedsores from increased production of urine and stool, swelling and breakdown of skin, and even pneumonia due to aspiration – the very problem they are intended to solve. Even though the patient is no longer being fed food or drink by mouth, PEG tubes do little to prevent aspiration. Sometimes this is because people continue to produce saliva, and this is inhaled. Overfeeding or weakness in the valve that separates the stomach and esophagus – swallowing tube — may be another cause of aspiration when formula trickles up the esophagus and into the trachea past a non-functioning epiglottis.
Understanding the Risks of End-Of-Life Eating
The decision to place a feeding tube in someone with advanced dementia, however, is a personal one. It should always be based on the individual’s wishes – which hopefully have been discussed before dementia made the conversation impossible — and may be influenced by many factors, including religious beliefs. If those wishes are not known, however, a decision based on their best medical interest would be to not place a tube. See below for discussion of options to provide food and fluid by IV in dementia.
What to do? First, it is important to recognize that aspiration is common, especially in elders, including those without dementia. And while it is almost too obvious to be said, the ability to enjoy the flavors and smells of food and drink is central to enjoying life – making the decision to place a feeding tube a very serious one. Why would anyone want to give up eating a great meal as life’s end approaches? Second, the consistency of food and fluid, and how it is eaten. can do a lot to help prevent aspiration. Pureed food is safer to eat and less likely to cause aspiration than more substantive forms of solid food, like chucks of meat or potato, and fluid thickened (usually with corn starch) to the consistency of maple syrup, called nectar-thick, is safer than regular “thin” fluids. Both make swallowing a slower and more easily controlled process and reduce – though not eliminate – the risk of aspiration.
Hospice Patients Are Offered Food and Fluid
In hospice, we offer food and fluid to everyone who wants and is able to eat and drink, regardless of risk of aspiration, so long as they understand and consent to the associated risks. Our nursing attendants are patient and skilled. Elders with dementia and risk of aspiration are fed while sitting upright – who eats while lying down?? – in small quantities – spoonfuls or even half spoonfuls at a time. Usually, though not always, aspiration is minimized or eliminated – and the food is enjoyed.
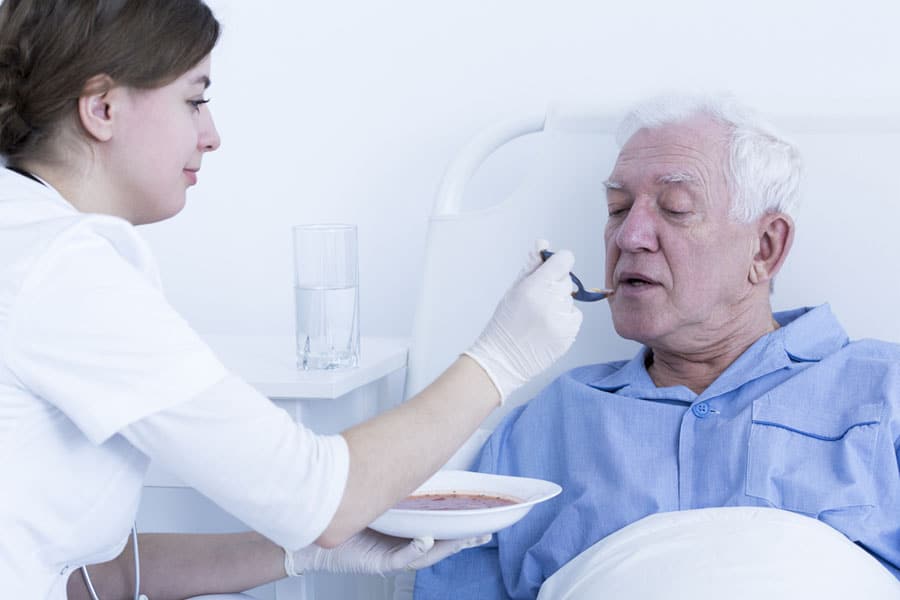
But what of people who are unable to eat or drink at all – in whom the problem is not aspiration, but a complete inability to swallow or hold food in the stomach?
What Is a Venting Gastrostomy Procedure?
Some of our patients have bowel obstruction, blockage of the intestine or stomach. This is most commonly due to advanced gastrointestinal or gynecologic malignancies, but can also be a complication of prior abdominal surgeries (the latter patients can sometimes have the obstruction relieved with more surgery). These patients can swallow just fine, but the food has nowhere to go once swallowed and is vomited back up again, sometimes violently. In cases like this, where surgery cannot reverse the blockage, a so-called venting gastrostomy can help. This fancy sounding procedure is quite simple. A tube, like a PEG tube, is inserted through the abdominal wall into the stomach, except now, instead of being used to put food into the stomach, it is used to drain food out of the stomach. People can enjoy the smells and favor of food and chewing and swallowing. The food and fluid they eat is simply drained out of the stomach through the tube after it is swallowed. I have more than once seen someone drink a cup of bright red cranberry juice and watched it come right back out through the tube seconds later. Once, a patient with a bowel obstruction told me her last wish was to eat raw oysters and vodka. I recommended a venting gastrostomy. A week later, we ate raw oysters and drank vodka together – after hours, of course.
And what of the nutritional and water requirements of people who can’t eat or drink – or whose food and fluid does not make it past their stomachs?
Quality of Life and IV Eating and Drinking
This is where the second question becomes important. What is the patient’s quality of life? The patient with a bowel obstruction who ate oysters and drank vodka was wide awake, fully aware of her situation, and lived life as fully as she could – visiting with friends and family, walking walks, enjoying media and books, much like everyone else. In her case, the provision not only of IV fluids, but complete intravenous nutrition was appropriate both medically and ethically. She had a PICC line – or peripherally-inserted central catheter, a type of long lasting IV – and was provided IV nutrition, called TPN or total parenteral nutrition, allowing her to stay alive and even relatively well for months. When her disease got worse, as the cancer that had spread through her body progressed, and as the quality of her life declined, the use of TPN became less helpful. She soon needed opioid analgesics for pain and sedatives for restlessness and drifted into unconsciousness. At this point, TPN became a liability, causing problems with increased volume of stool and urine, and associated increased bedside care needs that worsened her agitation, and a lot of saliva, causing coughing and choking. Now, there was no medically sound indication for IV fluid or TPN, and it was stopped – in keeping with her wishes and those of her family. She died peacefully soon after.
The Case Against IV Nutrition for Advanced Dementia Patients
The decision to provide intravenous nutrition and water to people with advanced dementia, on the other hand, is trickier. As was described in the discussion about feeding tubes, the quality of life in very advanced dementia is often poor – although this assessment is entirely subjective. The unfortunate patient with advanced dementia is bed bound, unable to eat, at such high risk of aspiration as to making eating impossible, completely dependent on others for cleaning and toileting, and profoundly cognitively impaired – unable to speak or understand spoken words, alive by virtue largely of having a pulse, blood pressure, and spontaneous respirations. IV fluid or TPN will keep a demented elder alive, as just defined, but the qualities usually associated with enjoying life, which may be as minimal as being just aware enough of and able to communicate in some way with loved ones, are entirely absent. To subject someone confronted by that horrific dilemma to IV fluid, and associated bedsores, swelling, increased secretions of saliva and aspiration, pneumonia, and repeated hospitalizations, is not a decision to be taken lightly and, in hospice, we recommend against it.
We hope this has been helpful. Keep your eye on the Connecticut Hospice blog for more information on topics relevant to people with advanced illness and their loved ones.
Further reading: Nutrition Concerns for Terminal Patients