
Honoring Our Legacy: Florence Wald and Hospice Care Over the Years
When one enters The Connecticut Hospice, it becomes almost immediately clear what a nurse-centric place it is. There’s a reason for that, and her name is Florence Wald. She was our founder, often called the Mother of Hospice in America.
In 1974, Florence Wald Founded The Connecticut Hospice as America’s first Hospice
For many years, the nurses have asked for a picture of our founder on the inpatient floor. Through the good graces of two retired Connecticut Hospice nurses, Gen O’Connell and Dianne Puzycki, and portrait painter, Angela Rose Agnello, (daughter of staff nurse), we unveiled the portrait of Florence Wald on the second floor yesterday, to great applause.

We have written elsewhere about our history, and the long list of our accomplishments, but it’s important also to understand just how Florence Wald changed the care of patients with terminal illnesses. After she spent time at the world’s first hospice in London, Saint Christopher’s, she returned with determination to alter the course of end of life care.
Florence Wald changed the way terminal cancer patients were treated
At that time, in the early 1970s, people often wouldn’t even say the word “cancer” out loud. Some of you remember when it was referred to as the “Big C”. There were even those who feared that cancer could be contagious, and were afraid to be too close to those who had it. Of course, in those days, the likelihood of survival was much lower. Sometimes, doctors didn’t tell patients, or families, what the course of the disease would be, or that person’s prognosis. This led to people dying without closure, or with survivors only beginning to process their grief.
For all these reasons, Ms. Wald decided early on to focus on the care of cancer patients. She was a force of nature, and was determined to change what many doctors and nurses considered standard practice at the time. Researchers can read many of Florence Wald’s papers, thanks to the Yale School of Nursing.
One of the key tenants of hospice care established by Florence Wald, was to provide holistic and comprehensive support and care for patients, caregivers, and family members.
Of particular concerns was what happened to those left behind, especially children of cancer patients. This might not be considered a good idea by many, but she got involved in the lives of the families, even taking some of the children home with her. She wanted them to have the comfort they weren’t getting in the medical system of that time.
In 1983, Connecticut Hospice was the first hospice to be reimbursed by Medicare.
Medicare set up what are now known as COP, Conditions of Participation, and they govern what hospice care needs to include. One of those requirements, 13 months of bereavement care for the survivors, is now practiced everywhere, and most likely came from those early principles espoused by Florence Wald.
Principles of hospice and palliative care were established at Connecticut Hospice in Branford.

Much of what we consider essential for death with dignity also harks back to those first patients. We now have a Plan of Care for everyone, and patients participate to whatever extent they can in planning for their end of life care. Doctors are now taught in medical school to have those difficult conversations, although many of them say that much more training is necessary. And, even though there is still a tension between the medical profession’s drive to keep patients alive, and the realities of the likely outcomes, we do see people choosing palliative care, when curative treatment becomes risky or speculative.
Cancer is not a verboten word anymore, but our tradition of treating the dying, no matter the cause, continues. We took wonderful care of AIDS patients in the early days of that scourge, and today we accept COVID-positive patients into our care. We try to give patients peace, comfort, freedom from pain, and closure, in whatever form that takes for them.
We honor Florence Wald in our continued pursuit of providing quality, comprehensive, and compassionate care for patients and their families.
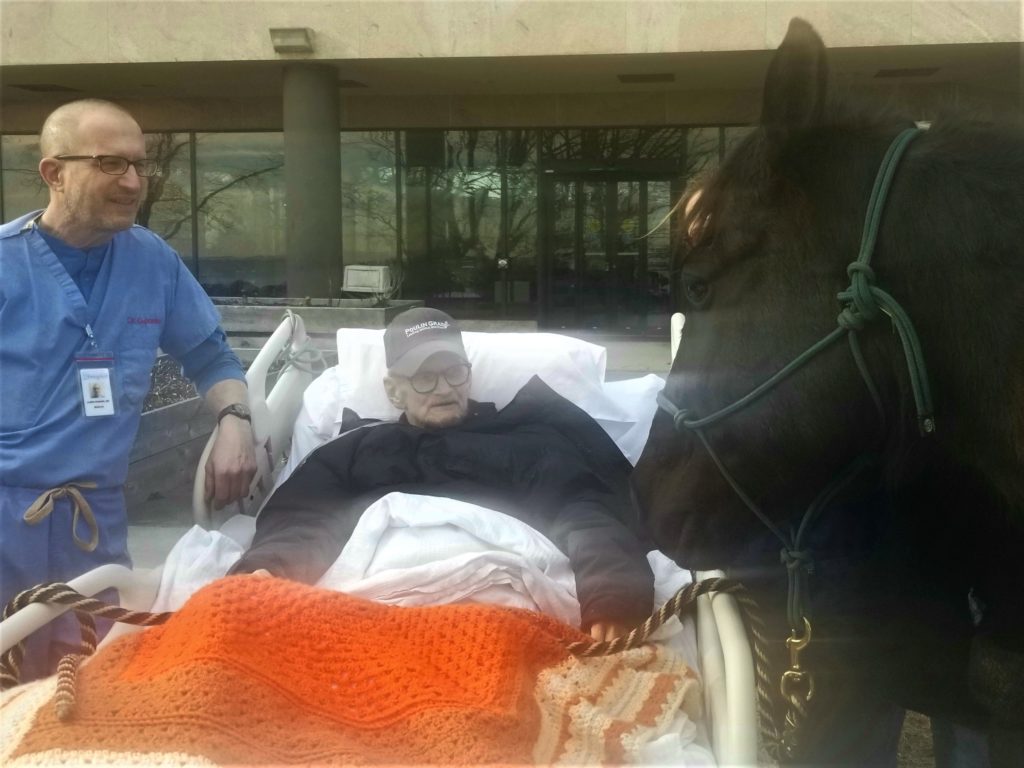
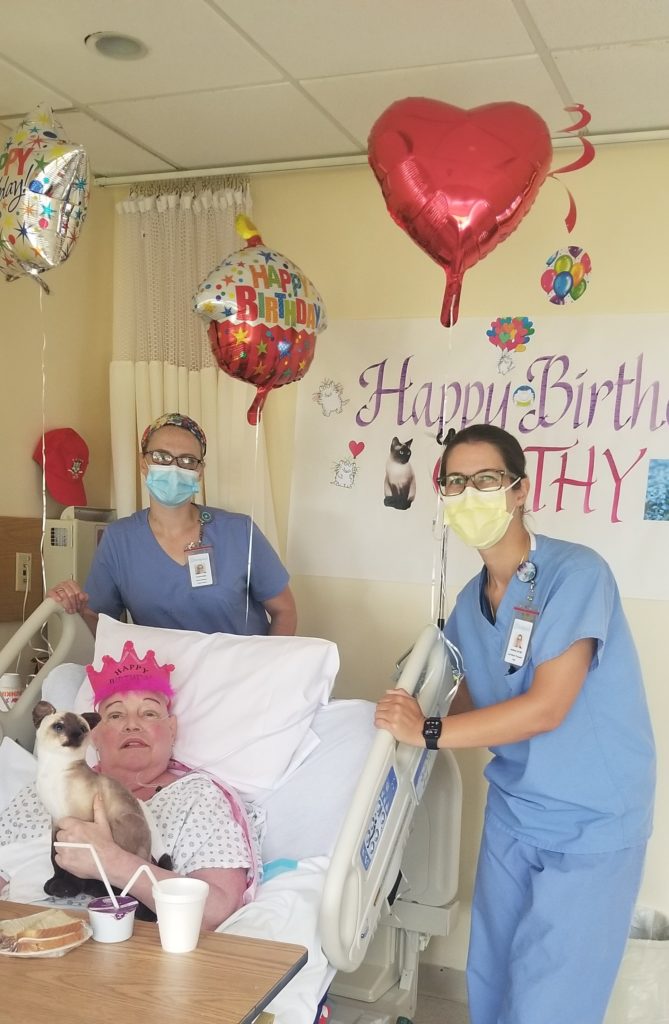
Florence would have been proud of us when we arranged for a dying man to say goodbye to his horse on our lawn, or when a social worker put another man’s feet into buckets of water pulled up onto his bed, so that he could feel the seawater one last time. Or, when a patient got to experience one last surprise birthday celebration, and share it with her family living on the other side of the country.
We are grateful for the wonderful legacy we have from Florence Wald and those early nurses who toiled alongside her. The world is a better place because of her work, and what better closure could there be to a life?





