August 12, 2025
Dementia and Hospice Eligibility
Understand Medicare’s hospice eligibility guidelines for dementia, including Alzheimer’s, related diagnoses, and required FAST score criteria.
December 10, 2024
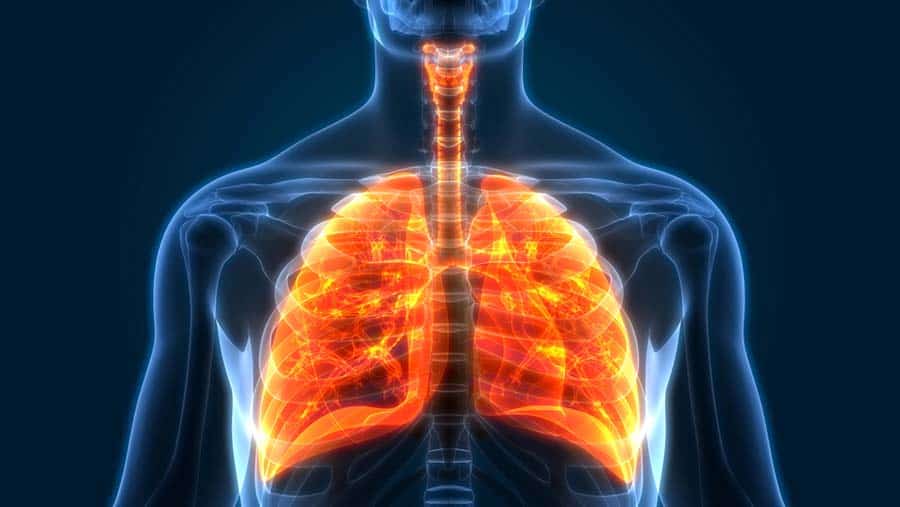
Intubation, Ventilation, and Tracheostomies in Hospice Care
Understanding Respiratory Failure Respiratory failure — the inability to breathe well enough to maintain life — is a…
November 5, 2024
Safely Crushing Medications for Hospice Patients
Learn safe methods for crushing medications for hospice patients, including which pills to avoid crushing and alternative options…
May 13, 2024
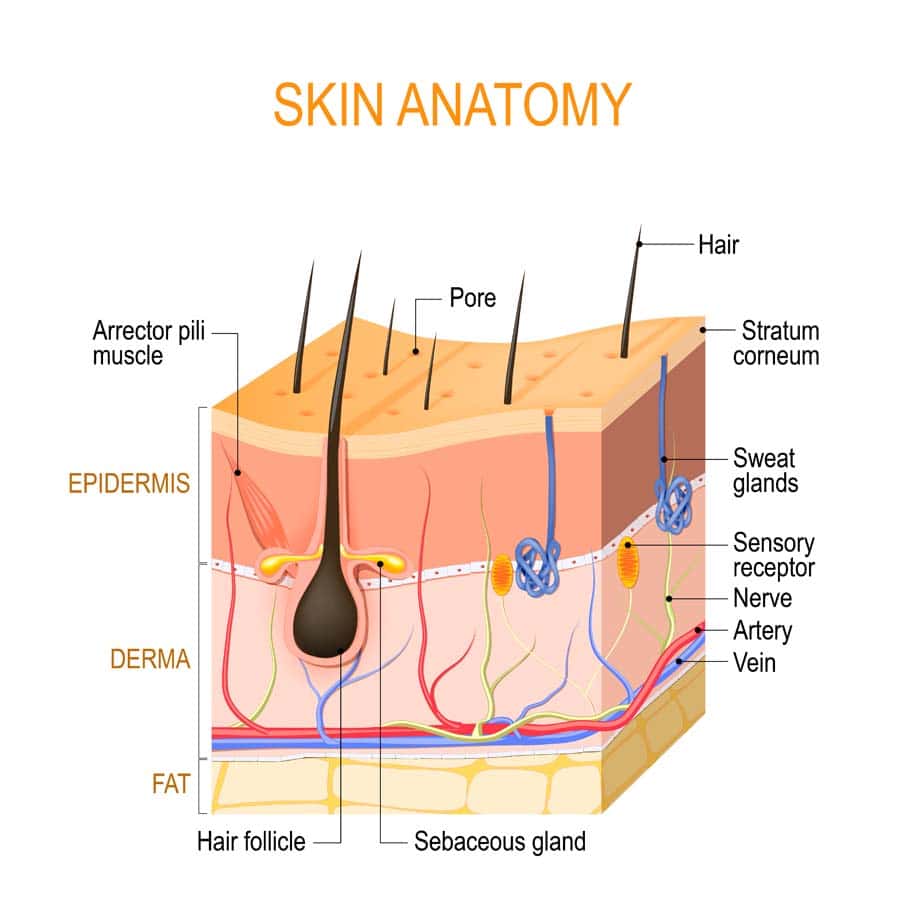
Skin Changes at the End of Life
A comprehensive guide to understanding skin changes at life's end. Learn causes, implications & strategies to alleviate distress…
April 8, 2024
New Outpatient Palliative Care Clinic
Find relief and support at Connecticut Hospice's new Outpatient Palliative Care Clinic. Expert symptom management and counseling available…
March 14, 2024
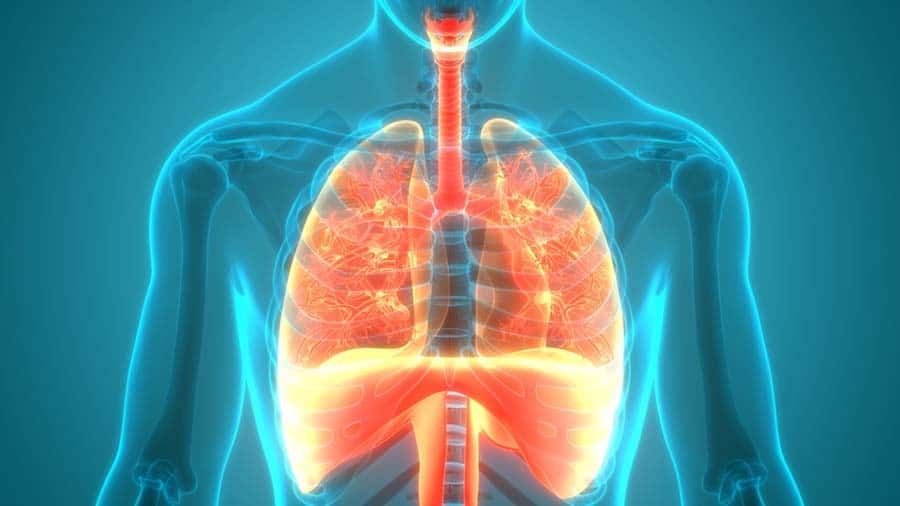
End-of-Life Breathing Patterns
What you need to know about breathing at the end of life: different breathing patterns, treatments, and compassionate…
February 14, 2024
Management of Agitation in Elders with Dementia
Strategies for managing agitation in hospice care. Understanding medication challenges and treatment options, to help preserve the dignity…
December 11, 2023
Nurturing Tomorrow’s Healers: Hospice Care Education
From clinical experiences to interdisciplinary rounds, discover how this institution shapes empathetic and skilled healthcare professionals in end-of-life…
Latest Posts
September 22, 2025
August 12, 2025
July 16, 2025