A Guide for Hospice Patients and Their Loved Ones

Much has been written about the best time to enlist hospice care, and there are certainly many medical and personal decisions to make. Since we see patients and families deal over and over with the same issues, we thought it might be useful to provide an overview of what they consider at such an emotional time. While the priorities may differ from person to person, a framework can help, especially at a time when it may be difficult to think calmly and concisely.
Be Open to Changes in Medical Directives as Illness Progresses
Since hospice care is very patient-centered, we should begin with the patient’s wishes.
Sometimes he or she is no longer able to verbalize desires, and sometimes those choices may change. For example, a wise doctor once gave a talk that can basically be summarized by stating that, when facing the possibility of death, most people choose life. That means that compromises in mobility, independence, and comfort, that may previously be rejected on principle, may be tolerated and even chosen, as illness progresses. Therefore, stated directives about health care choices may go out the window. If the patient is not competent, it becomes harder, and what he/she said at some earlier time may still be honored.
It is often true, as the end of life unfolds, that there are dips in ability followed by plateaus before another event takes the patient to a lesser state of functioning once again, which can be followed by a second plateau. This can go on for days, months, or years. The patient is often unhappy at the outset, but can become inured to the lesser capability, and even accepting. Someone who refused a walker or wheelchair, for instance, may use one when there is no practical alternative.
How to Make Decisions About Continuing Treatment
When speaking with the patient’s physician, the issue of further treatment can arise, and it can be hard to hear the real answer being given. Often, the easiest question for the doctor to answer, and the easiest to interpret, can be this: What would you do, if this were your parent, your spouse, or your child? Put that way, he/she is not being asked what to do, what is possible, or what the correct choice is. It is simply one person trying to judge the alternatives, based on what others might have chosen in similar circumstances. Asking about specific procedures is often better to frame in a statistical way, to avoid misunderstandings: What are the chances that this will work? What percentage of people get a meaningful extension of life from this?

Understanding Patient Wishes and Standards for Living
Once the medical side of the equation has been addressed, it is time to move onto preferences and feelings. The most basic question, then, to answer is this: What are your acceptable standards for living? This covers many things, from feeding tubes to mental capacity to chemotherapy. It is up to the patient to decide, whenever possible, how he or she wishes to proceed. Many choose to be DNR/DNI. (N.B. Although our inpatient facility takes admissions of those who wish to be resuscitated or intubated, we ourselves aren’t trained in those procedures, so call 911 like everyone else.) Others decide to forego further treatment, especially if it is painful or not working. Some even refuse food, particularly when the will to live has gone. Our job, not unlike that of family members, is to honor the patient’s wishes to the best extent possible. We strive to make someone comfortable and peaceful, and do not assume that we know what that means for any specific person.
Address Unfinished Business
That brings up the second question: Do you have any unfinished business, or last wishes? We hear so often about the proverbial bucket list, and many of us are busily checking things off that list now. However, there comes a point at which it seems not possible to fulfill further wishes. However, whenever possible, we as staff try to make those dreams a reality. That’s why we have weddings at Connecticut Hospice, either of patients, or of family members.
Fulfill Final Requests
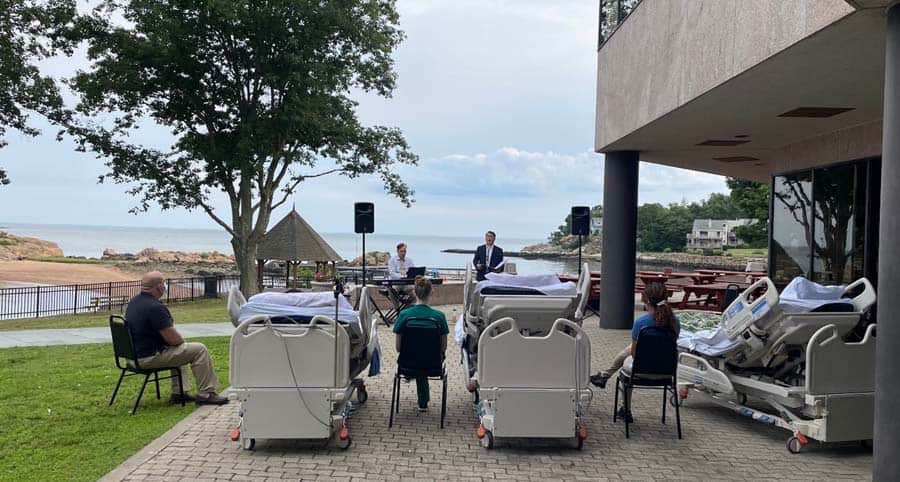
Sometimes, the request is to feel the ocean water on their toes one more time. In one such case, a social worker brought the patient’s bed to the water’s edge, and dumped buckets of water on his feet. He passed away within a couple of hours, a happy man. Going home one last time can be important, especially if there have been prolonged hospital or nursing home stays. That has been arranged for some people. Saying goodbye can mean seeing a beloved pet, and we have had them at Connecticut Hospice—most notably, a horse on the back lawn.


Offer/Receive Emotional Closure
Usually, the last wishes center around emotions, and forgiving or being forgiven.
We often tell families that it is important to say three things: I love you; I forgive you; and we will be ok if you leave us. So many people end up regretting that they stopped their loved one from talking about death, which can be an important part of the dying process. Letting him or her express final emotions can be very satisfying for them, and for the listener as well. Peace means many things to many people, but often it comes from letting negative emotions go, or apologizing or reconciling with someone. Helping that happen begins with asking the patient about closure.
Make Final Arrangements
If there is time, and desire, questions about funerals, burial or cremation, wills, or property may arise.
Again, it is hard, but important, to resist changing the subject, or saying that there is plenty of time to discuss things later. The patient knows his or her timetable best of all, and it can be a great comfort to settle some practicalities. Not infrequently, patients choose lesser levels of medication, even when it means more pain, in order to keep a clear mental status. Often that is for the purpose of having such discussions. They can even be prompted with your own question: Is there anything you want to tell me?

Allow the Patient to Discuss Their Death
For the many people who find this all difficult, they should realize that they are performing a great service is allowing tough questions to be answered. Providing someone with the gift of being heard is something you can do for him or her, when there is little else you can do. Even prompting memories allows the patient to realize that he or she will not be forgotten—a basic human desire, and one we are all likely to fulfill. Creating memories at the bedside can enrich those final days, and leave those mourning with smiles, even through tears.

Connecticut Hospice has always been an institution that honors final wishes, choices, and requests. We are grateful to be able to provide patients and families with the comfort that brings, and a privilege to have shared those moments with so many through the decades we have served our communities.