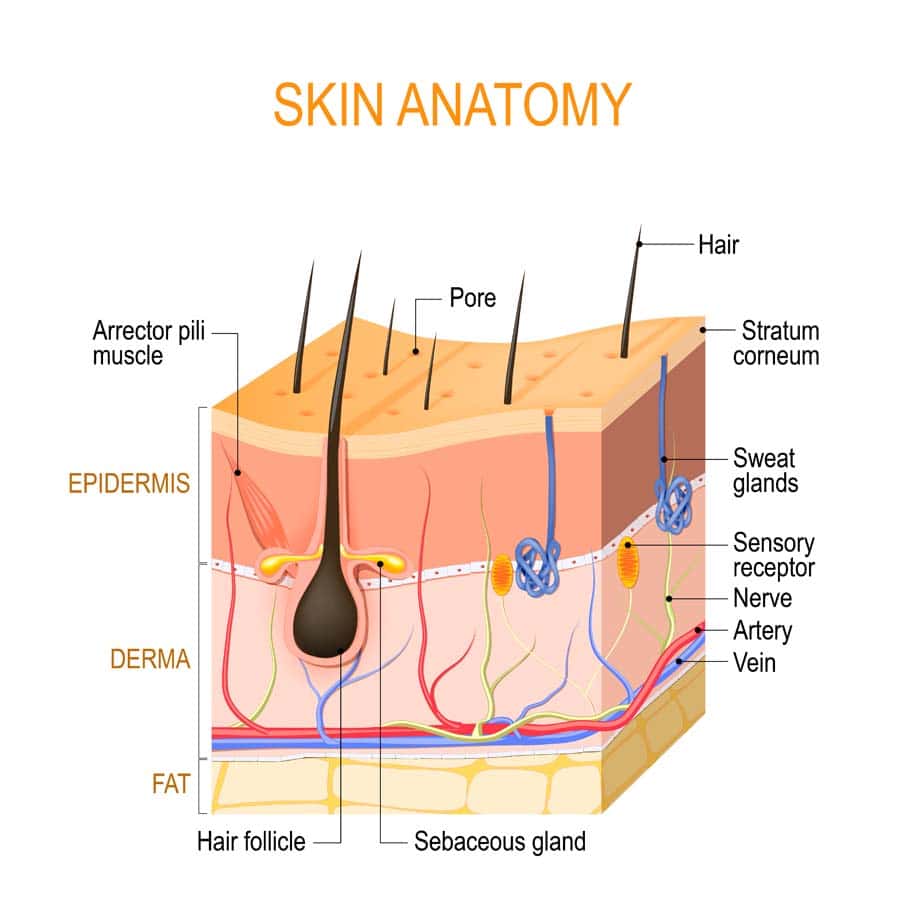
As we approach the end of life, our bodies undergo various transformations, both internally and externally. One of the most noticeable changes can be observed in our skin. Understanding these skin changes is crucial for caregivers, medical professionals, and loved ones to provide appropriate care and support. In this comprehensive guide, we will explore the common skin changes that occur towards the end of life, their causes, implications, and strategies for managing them effectively. Any and all of these changes are considered a normal part of the natural dying process.
Skin Changes in the Final Stages of Life:
- Pallor: As the body’s circulation declines, the skin may become pale or even bluish in color due to decreased oxygenation to the skin’s surface.
- Mottling: Mottled skin appears as blotchy patches of discoloration, often seen first in the extremities. It occurs due to reduced blood flow to the skin’s surface resulting in irregular patterns of pale and discolored areas. Mottling is a common occurrence in the last days or hours of life and is considered a normal part of the dying process.
- Dryness: Dehydration and decreased oil production can lead to dry, flaky skin, which may feel rough and tight to the touch.
- Bruising: Fragile skin and reduced clotting ability make individuals more susceptible to bruising, even from minor bumps or pressure. Bruises may appear more easily and take longer to heal as the body’s ability to repair damaged blood vessels diminishes. Bruising is also more easily caused when patients are on blood thinners or anticoagulants.
- Pressure Ulcers: Prolonged immobility can result in pressure ulcers, also known as bedsores, particularly in areas where bones are close to the skin, such as the heels, hips, and sacrum. These are nearly inevitable as the skin fails.
- Skin Tears: Thin, fragile skin is prone to tearing, especially during movement or handling.
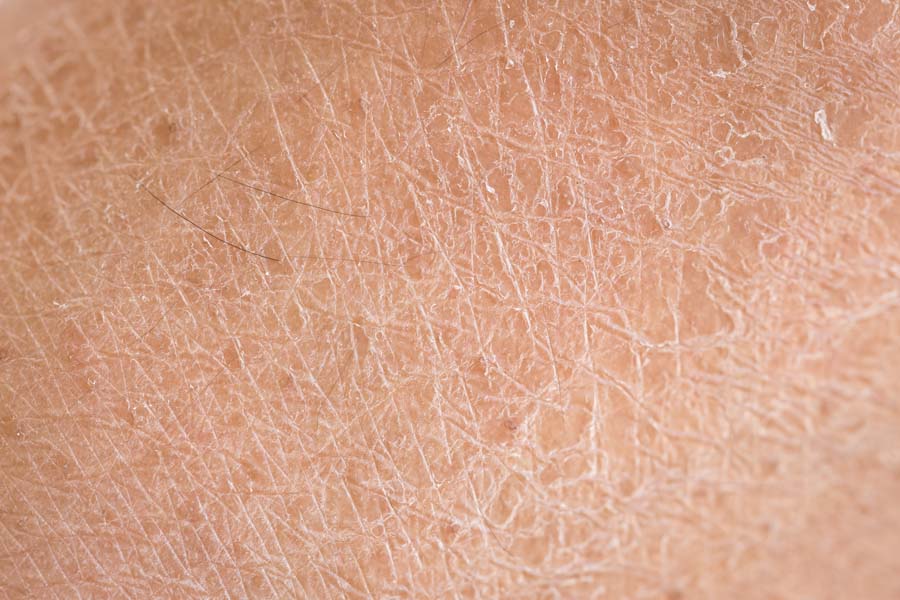
Contributing Factors to End-Life Skin Changes:
Circulatory Changes: Reduced blood flow to the skin contributes to pallor, mottling, and increased susceptibility to pressure ulcers. As the body’s systems begin to shut down, blood is redirected to essential organs, leading to decreased perfusion of the skin and other peripheral tissues.
Dehydration: Diminished fluid intake or inability to process fluids properly can lead to dry, cracked skin. Dehydration is common in the end-of-life stage due to decreased oral intake, increased fluid losses, and metabolic changes.
Nutrition: Poor nutrition, common towards the end of life, can impair skin health and delay wound healing. Malnutrition, along with underlying medical conditions, can weaken the skin’s structure and compromise its ability to withstand pressure and trauma.
Medications: Certain medications may affect skin integrity, moisture levels, and clotting mechanisms. For example, anticoagulants can increase the risk of bruising and bleeding, while diuretics may contribute to dehydration and electrolyte imbalances
Immobility: Limited mobility increases the risk of pressure ulcers and skin tears, as well as exacerbating circulation issues. Individuals who are bedridden or confined to a wheelchair are particularly susceptible to skin breakdown due to prolonged pressure and lack of movement.
Psychological and Emotional Impact of Skin Changes in Dying Patients
Skin changes can be distressing for both the individual nearing the end of life and their loved ones. Visible alterations in skin appearance may serve as a stark reminder of the person’s declining health and mortality. Discomfort and pain associated with skin issues can also exacerbate emotional distress and affect overall well-being. It is important to discuss these changes with your medical provider and for the medical team to reassure and educate loved ones that these changes are a natural part of the dying process. Open and honest communication with the individual and their caregivers is essential to address concerns and provide reassurance. Emotional support, including validation of feelings and offering comfort, can help alleviate distress related to skin changes. Collaboration with healthcare professionals, including nurses, wound care specialists, and palliative care teams, is vital for comprehensive holistic care when it comes to managing these skin changes at end of life.
Strategies for Managing End of Life Skin Changes:
- Moisturize: Regular application of emollients or moisturizing creams can help alleviate dryness and maintain skin integrity.
- Positioning: Proper positioning, with frequent changes to relieve pressure points, can prevent some pressure ulcers.
- Gentle Handling: Handle the individual’s skin with care to minimize the risk of skin tears and bruising.
- Nutrition and Hydration: Ensure adequate fluid intake and a balanced diet to support skin health and healing.
- Pain Management: Address any discomfort or pain associated with skin changes through appropriate pain management techniques. Use analgesic medications as prescribed and consider non-pharmacological interventions, such as massage or heat therapy, to alleviate pain and promote relaxation.
- Wound Care: Follow recommended wound care protocols for pressure ulcers, skin tears, and other skin injuries to promote healing and prevent infection.

Dignity and Comfort in End-of-Life Care
Providing dignified and comfortable care for individuals experiencing skin changes at the end of life is paramount. Respect for the individual’s autonomy, privacy, and preferences should guide all aspects of care, including skin care routines and interventions. Encourage the individual or family members to participate in decisions regarding their care to promote a sense of control and agency.
Maintaining privacy and modesty is essential when addressing skin changes, as individuals may feel vulnerable or self-conscious about their appearance. Respectful communication and sensitivity to cultural and personal beliefs can help preserve the individual’s dignity and promote a positive care experience. Additionally, incorporating rituals or practices that hold significance for the individual, such as religious ceremonies or personal grooming habits, can enhance their sense of well-being and spiritual comfort.

Skin Changes Are a Natural Part of Dying
By understanding the causes and implications of these changes and implementing appropriate strategies, caregivers and loved ones can help maintain the individual’s comfort and dignity during this challenging time. Through open communication and compassionate care, we can support those nearing the end of life in their journey with grace and dignity.
Understanding Skin Changes Enhances Quality of Life
Understanding and addressing skin changes at end of life is essential for providing holistic care to individuals nearing the end of their journey. These changes, ranging from pallor and mottling to pressure ulcers and skin tears, are natural manifestations of the body’s decline and require thoughtful management to maintain comfort and dignity. By recognizing the contributing factors, implementing appropriate interventions, and fostering open communication and support, caregivers, medical professionals, and loved ones can help alleviate distress and enhance quality of life for those in their care.
As we navigate the complexities of end-of-life care, it is crucial to uphold the principles of dignity, compassion, and respect for the individual’s autonomy and preferences. Each person’s journey is unique, and tailoring care approaches to meet their specific needs and wishes is paramount. Through this understanding, we can ensure that individuals facing skin changes at the end of life receive compassionate and comprehensive care that honors their humanity and affirms their inherent worth. Together, we can embrace the journey with empathy and grace, providing solace and support to those embarking on life’s final chapter.






