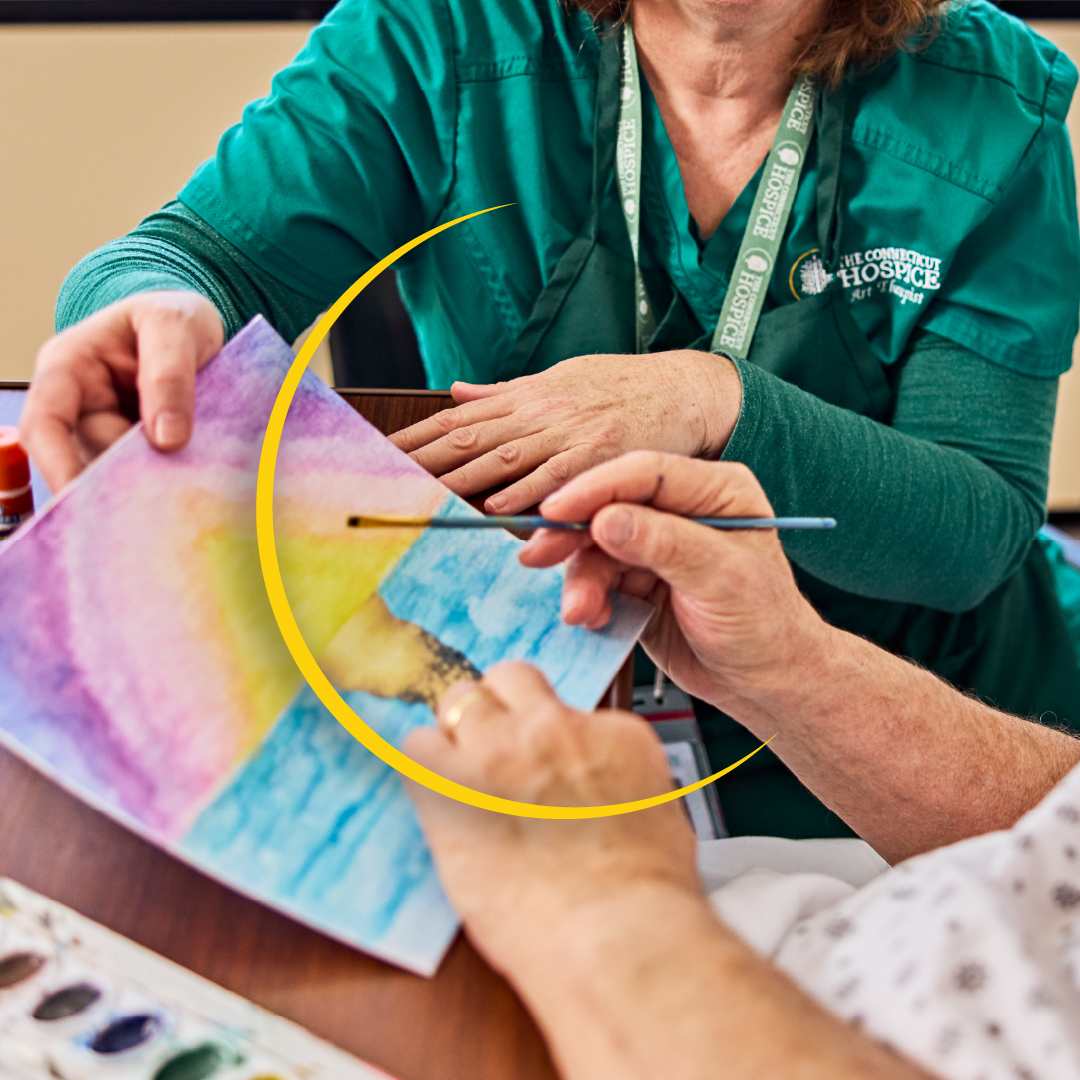
One of the hardest questions families face is, “When is it time to call hospice?”
There isn’t a single moment when the answer becomes obvious. More often, it’s a series of changes: the most recent hospital visit might feel different from the last one. A loved one may be sleeping more, eating less, and needing more help than they did just weeks ago. Treatments that once seemed helpful may now feel exhausting or burdensome.
Many people begin searching for signs that hospice is needed because something has shifted, even if they can’t fully explain how. This guide is here to help you understand what those changes may mean and recognize them more clearly. Learning what hospice does and how decline is typically assessed can help you make a thoughtful, informed decision about next steps.
For healthcare professionals seeking detailed clinical criteria, please read our blog on hospice eligibility and documentation guidelines.
Important Takeaways
- Hospice is about a larger picture, not one symptom. A series of changes over time often signals when it may be time to call hospice, rather than a single event.
- When treatment no longer aligns with a loved one’s goals, hospice care shifts the focus to comfort, support, and quality of life.
- You don’t have to be certain to start the conversation. If you’re noticing signs that hospice is needed, reaching out can help you understand your options and next steps.
What Does Hospice Do?
Hospice care is specialized end-of-life care for people facing a life-limiting illness, typically with a prognosis of six months or less. Rather than pursuing curative therapies aimed at treating disease, hospice care prioritizes comfort, dignity, and quality of life.
At The Connecticut Hospice, care extends beyond medical treatment. We support patients and the people who love them, addressing physical symptoms as well as emotional, social, and spiritual needs. An interdisciplinary team comprising nurses, physicians, social workers, aides, chaplains, and therapists collaborates to create a plan centered on what matters most to the patient and family.

Understanding When to Call Hospice
It’s one of the most common questions we hear: “How do we know it’s time for end-of-life care?”
Hospice is appropriate when treatments aimed at curing an illness are no longer effective, no longer desired, or are creating more burden than benefit. It may also be time to call hospice when comfort, quality of life, and support become the priority, rather than curing a disease or slowing its progression.
Know that you don’t have to be certain before reaching out. A conversation with our Admissions Department can help you understand options and timing without committing to a plan of care.
Physical Signs That Hospice May Be Needed
Although every illness follows its own path, there are common indicators of decline that suggest it may be time to explore hospice care.
|
Indicator |
Signs You May Notice |
|
Medical Instability |
|
|
Uncontrolled Symptoms |
|
|
Physical Decline |
|
|
Behavioral or Neurological Changes |
|
|
Loss of Independence |
|
These changes can appear gradually: a loved one’s clothing may fit differently, or their meals may become smaller. A once-independent person might now need assistance getting out of a chair.
One sign alone does not necessarily mean hospice is needed. However, when several of these changes occur together or progress over time, it may be appropriate to begin a conversation.
Emotional and Behavioral Changes at the End of Life
Families often notice emotional or cognitive changes before they recognize physical decline.
|
Indicator |
Signs You May Notice |
|
Emotional and Social Withdrawal |
|
|
Cognitive Changes |
|
|
Shifts in Goals of Care |
|
|
Life Review and Closure |
|
|
Changes in Communication or Perception |
|
These experiences can be deeply personal. Hospice teams are trained to support families through them with compassion and respect.

Clinical Guidelines Doctors Use
Physicians rely on established medical criteria when determining hospice eligibility. Under the Medicare hospice benefit, a doctor must certify that a patient is likely to have a life expectancy of six months or less if the illness progresses typically.
Clinical indicators often include:
- Documented decline in functional status
- Increasing dependence in two or more activities of daily living (ADLs), such as bathing, dressing, feeding, or transferring
- Progressive weight loss
- Recurrent hospitalizations related to the terminal illness
- Disease-specific markers, such as worsening heart failure, advanced COPD, late-stage dementia, metastatic cancer, or other serious conditions
Tools such as the Palliative Performance Scale (PPS) or the Karnofsky Performance Status (KPS) help clinicians measure functional decline. Generally, scores below 70% indicate a significant reduction in independence and may support hospice eligibility. These assessments are not meant to reduce a person to numbers; they simply help physicians understand when hospice support is medically appropriate.
What Gradual Decline Can Look Like
Every person’s experience is different. But over time, families often begin to notice changes like these as signs that hospice is needed. When they occur together and continue to progress, they often signal that the body is declining and that comfort-focused care may be appropriate.
|
Weight Loss A patient who is now mostly bed-bound may no longer be able to stand on a scale. However, even without an exact number, change is visible. Over several months, their arms and legs have become thinner, their wedding rings have been slipping more easily, and their clothing has appeared to be “falling off of them.” |
Loss of Appetite Meals become smaller and less consistent. A patient may have four to six child-sized meals each day. Instead of full portions, they may take just a few bites, finishing only a quarter of what’s offered. For example, breakfast might be 2 slices of bacon and a bit of grits; lunch might be a few spoonfuls of soup or part of a nutritional supplement shake. |
|
Functional Decline A patient who was independent just a few months ago may now need help bathing, dressing, or walking safely. A walker may be required for short distances. Activities of daily living (ADLs) that once felt routine now require assistance. The shift from driving, working, or managing a household to needing support can happen more quickly than families expect. |
Changes in Sleep Patterns Sleep often increases. A patient may rest eight to ten hours at night and still nap for several hours during the day. Sitting upright in a chair for more than an hour may lead to dozing. Families sometimes notice that, within weeks, a patient goes from experiencing nighttime restlessness or difficulty sleeping to spending more time asleep than awake. |

Earlier Is Often Better
One of the most common reflections we hear from families is that they wish they had called sooner.
Hospice is not only for the final days of life. When services begin earlier in the course of the decline, patients and families often experience:
- Better symptom management
- Fewer crisis hospital visits
- More time at home
- Stronger emotional and practical support
Hospice can also create space for conversations, closure, and presence that may not happen during repeated medical emergencies.
Unsure When to Call Hospice? Start With a Conversation
If you’re wondering when to call hospice, that alone is often a sign that it may be time to ask.
You do not need to have everything figured out. A phone call allows you to speak with a knowledgeable professional who can review your loved one’s situation, answer questions, and help you explore potential next steps. Reaching out is not a commitment; it’s simply a step toward understanding your options and making decisions with confidence.
The Connecticut Hospice is here to provide clear information, thoughtful guidance, and compassionate end-of-life care, whenever it’s needed. When the time feels right, we are here to help.