Please view our updated COVID-19 guidelines and visiting procedures →.
Music has long been recognized for its ability to evoke emotions and memories, making it a powerful tool in therapeutic settings. For dementia patients, music therapy offers a unique and effective way to enhance quality of life, improve cognitive function, and reduce behavioral issues.
This non-invasive treatment harnesses the universal language of music to connect with patients on a deep emotional level, providing comfort and joy in ways that traditional therapies often cannot. In this article, we will explore the numerous benefits of music therapy for dementia patients, highlighting its impact on mental, emotional, and physical well-being.
Music therapy involves a structured program where trained therapists use music to address physical, emotional, cognitive, and social needs of individuals. For dementia patients, this therapy leverages the brain's response to music to stimulate memory, improve mood, and facilitate communication. The power of music lies in its ability to activate multiple brain regions simultaneously, providing a unique and effective form of therapy.
Music therapy can significantly enhance communication skills in dementia patients, providing a valuable tool for expressing thoughts and emotions. Here's how it helps:

Overall, music therapy offers a multifaceted approach to improving communication in dementia patients, making it an invaluable part of their care and treatment.
One of the most significant benefits of music therapy for dementia patients is its ability to enhance cognitive function. Music engages the brain's memory centers, often evoking memories and emotions from the past. This engagement can help maintain and even improve cognitive abilities. Studies have shown that listening to music, especially songs from a patient's youth, can trigger memories and improve recall. This stimulation helps keep the brain active, potentially slowing the progression of cognitive decline.
For instance, it's been found that dementia patients who participated in music therapy showed significant improvements in cognitive function compared to those who did not. The rhythmic and repetitive aspects of music provide a structured framework that can help patients with memory retrieval and organization of thoughts.
Music therapy significantly enhances the emotional and psychological well-being of dementia patients. Music has a profound impact on mood, often eliciting strong emotional responses. For dementia patients, who may experience anxiety, depression, and agitation, music therapy provides a source of comfort and joy.
Listening to music or participating in musical activities can elevate mood, reduce anxiety, and alleviate symptoms of depression. The emotional connection to music can also help patients express feelings that they might not be able to articulate otherwise. Singing, for instance, can provide an emotional release and foster a sense of connection with others.
Chronic stress and anxiety can have detrimental effects on brain health and overall well-being. Music therapy offers a powerful tool for reducing stress and anxiety in dementia patients. The calming effects of music can lower levels of stress hormones like cortisol, providing a sense of relaxation and peace.
Listening to soothing music or engaging in relaxing musical activities can help alleviate anxiety and promote a calm environment. This relaxation is particularly beneficial for dementia patients, who may experience heightened anxiety and agitation due to their condition.

A licensed, board-certified music therapist in Connecticut possesses the specialized training and expertise necessary to provide effective music therapy for dementia patients. Utilizing personalized assessments and tailored treatment plans, these professionals use music to address the cognitive, emotional, and physical needs of their patients, enhancing their quality of life in significant ways.
The process begins with a thorough assessment of the patient’s cognitive abilities, emotional state, and physical health. The therapist also gathers information about the patient’s musical preferences and history, which plays a critical role in developing an effective treatment plan. This personalized approach ensures that the therapy addresses the unique needs of each patient, focusing on specific goals such as improving memory recall, reducing anxiety, and fostering social interaction.
Engaging music activities are at the heart of effective music therapy for dementia patients, providing a dynamic and multifaceted approach to care. Licensed music therapists utilize a variety of activities tailored to the individual needs and preferences of each patient. These activities include listening to familiar music to evoke memories and comfort, singing along to favorite songs to enhance verbal skills and mood, and playing simple instruments like drums or tambourines to improve motor coordination and provide a non-verbal outlet for expression. Movement-based activities, such as dancing or rhythmic exercises, stimulate physical health and reduce agitation, while songwriting and lyric analysis offer opportunities for emotional expression and cognitive engagement.
Playing songs from the patient’s past can evoke strong emotional responses and trigger memories. This engagement helps improve cognitive function and provides a sense of comfort and familiarity. For instance, a patient might recall specific events associated with a particular song, which can enhance their ability to communicate and interact with others.
Encouraging patients to sing along to their favorite songs can enhance verbal communication skills and elevate mood. Singing familiar lyrics can help with language retention and recall, which is particularly beneficial for patients struggling with speech.
Using simple instruments like drums, tambourines, or maracas allows patients to participate in rhythmic activities, improving motor skills and coordination. Instrument play also provides a non-verbal way for patients to express themselves, which can be especially helpful for those with advanced dementia.
Incorporating movement, such as dancing or rhythmic exercises, can enhance physical health and coordination. Movement to music stimulates the brain and can reduce agitation and restlessness, helping patients to feel more relaxed and engaged.
For patients with more advanced cognitive abilities, songwriting and discussing song lyrics provide an outlet for emotional expression and foster deeper connections with caregivers and family members. This activity can stimulate critical thinking and creativity, offering a therapeutic benefit beyond mere enjoyment.
Music therapy offers a holistic and effective approach to supporting dementia patients, providing numerous cognitive, emotional, and social benefits. By engaging the brain, enhancing communication, reducing stress, and encouraging social interaction, music therapy can significantly improve the quality of life for dementia patients. As awareness of its benefits grows, music therapy is becoming an increasingly integral part of dementia care, offering hope and comfort to patients and their families.

In the ever-evolving landscape of medical education, institutions that prioritize hands-on experience, interdisciplinary collaboration, and compassionate care are invaluable. The Connecticut Hospice stands out as a beacon of excellence, offering a myriad of educational opportunities for pre-med students, medical students, residents, and fellows. This blog post will delve into the educational programs provided by The Connecticut Hospice through the John D. Thomas Institute and shed some light on how they contribute to the development of well-rounded and empathetic healthcare professionals.
Before delving into the educational offerings, it's essential to understand the foundation upon which The Connecticut Hospice stands. Established in 1974, it holds the distinction of being the nation's first hospice. Its mission revolves around providing patient-centered, end-of-life care rooted in compassion, dignity, and respect. This commitment to holistic care forms the backbone of the educational opportunities offered.
The John D. Thompson Hospice Institute for Education, Training and Research, Inc. (JDT Institute), the educational ally of Connecticut Hospice, was established in 1979, when it gave its first educational conference. The JDT Hospice Institute is a vehicle for sharing the hospice philosophy with all who desire to improve the quality of care for patients (and their loved ones) experiencing an irreversible illness. It offers opportunities for students, health care professionals, administrators, caregivers, and the lay community to learn, and gain experience and skills in hospice care.
At the core of good hospice care is the interdisciplinary team approach. Every patient is cared for by a team that includes medicine, nursing, social work, spiritual, bereavement, pharmacy and volunteers. The team ensures the patient receives care at the physical, mental, and/or emotional levels, if and when needed during their journey. Connecticut Hospice offers clinical rotations in medicine, nursing, social work, and pharmacy.
Traditionally the first milestone in the long journey to becoming a practicing healthcare provider is usually shadowing other providers. Here at Branford, we offer extensive shadowing opportunities. Students can observe seasoned healthcare professionals navigating the challenges of end-of-life care, learning not only medical procedures but also the nuances of compassionate communication both in our inpatient unit as well as with our homecare team. Recognizing the importance of early exposure to hospice and palliative care, The Connecticut Hospice offers pre-med programs designed to ignite the interest of aspiring healthcare professionals and expose them to the realities of practicing medicine in our current healthcare system as well as mentor them to the requirements of applying to graduate professional programs.

Students approved to complete clinical hours at The Connecticut Hospice are afforded a unique and enriching experience. Although many come from schools in the Northeast, the opportunities to rotate here are open for all institutions across the country. The institution recognizes the importance of exposing future physicians, nurses, social workers, art therapists, music therapists and pharmacists to end-of-life care, fostering empathy, and refining communication skills. Through structured programs, students have the chance to shadow experienced practitioners, and engage in patient care activities under the guidance of experienced mentors. This hands-on experience allows them to apply theoretical knowledge in a real-world setting, honing their clinical skills and deepening their understanding of the unique challenges in end-of-life care.
Throughout COVID, and the nursing shortage, Connecticut Hospice worked with area nursing programs to provide clinical practice hours that were standing in their way of graduating and joining the dwindling nursing pool. Yes, it is about teaching how to provide good hospice and palliative care, but it is also about sharing the importance of both hospice and palliative care in the cycle of terminal illness.
The Connecticut Hospice places a strong emphasis on interdisciplinary collaboration. Learners here actively participate in rounds that bring together physicians, nurses, social workers, and other healthcare professionals. This approach provides a holistic view of patient care, fostering an understanding of the diverse skills required in end-of-life medicine.

For medical residents seeking to specialize in palliative care or related fields, The Connecticut Hospice offers comprehensive clinical exposure to end of life medicine. Residents may come from any ACGME accredited program and specialty. These programs provide a structured curriculum that combines clinical experience, research opportunities, and mentorship in a variety of inpatient and outpatient settings. Rotating residents at The Connecticut Hospice benefit from a diverse range of clinical experiences. From managing complex symptoms to leading family meetings, residents are actively involved in the care of patients facing life-limiting illnesses. This exposure equips them with the skills necessary for providing compassionate and effective end-of-life care.
Students earning an advanced degree in nursing, social work, art therapy, music therapy or pharmacy spend a significant amount of time at Connecticut Hospice, quickly becoming a member of the care team and gaining unique experiences from collaborating care.
Social Workers pursuing a Masters spend their entire final year with us, allowing them the opportunity to learn from a seasoned social worker how to best guide a patient and their family through one of the most stressful events of life, death of a loved one. There are so many factors to consider when caring for a family unit, especially when death is at the core. It takes time for a social worker to become comfortable with the unique needs of a hospice population and the extended time allows for learning and experiencing from the seasoned social worker.

The JDT institution encourages learners across the spectrum of academia to engage in research projects that contribute to the evolving field of palliative care. By collaborating with experienced researchers and faculty members here at the Connecticut Hospice, learners get the opportunity to explore innovative approaches to symptom management, psychosocial support, and ethical considerations in end-of-life care and receiving the structured mentorship to pursue their own individual projects.
Every PharmD candidate who completes a month-long rotation with Connecticut Hospice’s onsite Pharmacy Department is required to present findings on a pharmacological topic selected prior to the start of their rotation. The findings are presented on the student’s final day to members of the interdisciplinary team who were all part of the learning experience. The collaboration between a student and those with heavy experience can create something great.
Mentorship plays a pivotal role in the residency programs at The Connecticut Hospice. Our learners work closely with our seasoned professionals who provide guidance not only in clinical matters but also in navigating the emotional and ethical dimensions of palliative care, as well as preparing for the next step in their own professional journeys.
If clinical medicine isn’t desired, The Connecticut Hospice also can offer unique individualized internships with our senior management and executive teams. Rotating through our non-profit and working directly with our executives provides the learner with a special opportunity to collaborate closely on business development plans and network with regional partners.
The Connecticut Hospice's offers tailored programs and educational workshops that cover the basics of palliative care, hospice care, pain management, and the psychosocial aspects of end-of-life care. These workshops serve as a bridge between classroom learning and practical application in the community. We offer these experiences and lectures to our community partners and travel to them to deliver these interactive and informative sessions.

In addition to the above, The Connecticut Hospice offers a robust and enriching volunteer experience. These hands-on experiences allow each person to donate their time and/or talent to our patients in a multitude of ways. Each new academic year provides Connecticut Hospice with more than 75 medical students looking to volunteer to gain experience working with patients and families. These future healthcare providers create a positive energy that fills the building. In addition to these medical students, Connecticut Hospice is always in need of volunteers to share their talents with us. If you or your organization is interested in volunteering, please reach out to our Director of Volunteers at [email protected].

The educational opportunities offered by The Connecticut Hospice form a critical component of the institution's commitment to advancing the field of hospice and palliative care. No matter what a student’s ultimate position is in healthcare, Connecticut Hospice encourages them to take the unique experiences offered at America’s first hospice to enable them to be the best they can be throughout their career. By combining hands-on experiences, interdisciplinary collaboration, and a commitment to compassionate care, The Connecticut Hospice is shaping the next generation of healthcare professionals who will navigate the complexities of end-of-life medicine with skill, empathy, and resilience. As we look toward the future of healthcare, the lessons learned at The Connecticut Hospice serve as a guiding light for those dedicated to providing dignified and compassionate end-of-life care.
For more information on clinical rotations at Connecticut Hospice, email [email protected].
Opioids are a critical means of relieving pain and shortness of breath in people with serious illnesses. While non-opioid analgesics such as acetaminophen (Tylenol) and ibuprofen (Advil, Motrin) may partially or fully relieve mild to moderate pain, these agents have no effect on shortness of breath, and opioids are usually required for more severe pain.
Before describing different opioids and how and when to use them, let’s review some broadly held concerns about this class of medication.
First, and perhaps most importantly, is the belief that opioids cause respiratory depression and hasten dying. There is no question that opioids can slow respiration, especially if used incorrectly or given in high doses. However, the reality is that respiratory depression with opioids in the setting of life-limiting illness is rare. A well-conducted study of opioids in cancer patients with shortness of breath conducted 30 years ago showed that these medications were effective in relieving symptoms and resulted in no significant respiratory depression (Bruera E, MacEachern T, Ripamonti C, Hanson J. Subcutaneous morphine for dyspnea in cancer patients. Ann Intern Med. 1993;119(9):906–907). Another study, conducted in 2002, showed that opioids are also safe and effective for the treatment of shortness of breath or pain in patients with chronic obstructive pulmonary disease and heart failure (Jennings AL, Davies AN, Higgins JP, Gibbs JS, Broadley KE. A systematic review of the use of opioids in the management of dyspnoea. Thorax. 2002;57(11):939–944).
Unfortunately, the belief that opioids hasten dying persists among both medical and nursing professionals and the public at large. The physicians and nurse practitioners at The Connecticut Hospice, Inc. are highly experienced in the safe use of opioids, making this concern unnecessary for the care of you or a loved one. While the use of very high doses of opioids at the very end of life in patients who are not conscious may result in some respiratory slowing, this is never the reason they are used, which is solely to effect relief of pain and shortness of breath in patients who are suffering.

Another widely held perception about opioids is that they necessarily cause addiction, or opioid use disorder (OUD). Unfortunately, as with beliefs about respiratory depression, the consensus around the medical use of opioids and OUD is nuanced and merits closer examination.
CDC Guidelines: Shaping the Landscape of Opioid Use
First, there is no question that the inappropriate use of opioids in the medical setting, especially in the 2000s, contributed to the spread of OUD and the opioid epidemic, which in 2021 took the lives of 106,000 of our friends, neighbors, and family members. Aggressive marketing of opioids for medical use and the overprescribing of opioids for both acute pain (“acute” meaning of recent onset, such as for a broken bone or dental problem) and chronic pain clearly resulted in OUD and death in some patients. Partially in response to this, the CDC (Centers for Disease Control) issued guidelines in 2016 on the use of opioids for pain. While the report made clear that the evidence on harm related to the medical use of opioids was less than optimal, they recommended nonopioid pharmacologic therapy as preferred for chronic pain, with numerous caveats and warnings for those patients with chronic pain who were prescribed opioids. For people with acute pain, no more than a 3-to-7-day supply of opioids was recommended. A wave of legislation and regulatory actions on the medical use of opioids followed, resulting in an almost 50% decline in opioid prescribing from 2016 to 2019. The CDC updated these guidelines in 2022, still recommending non-opioid therapy for chronic pain, though also stating, “No validated, reliable way exists to predict which patients will experience serious harm from opioid therapy and which patients will benefit from opioid therapy.” The report softened its position regarding acute pain, stating, “When opioids are needed for acute pain, clinicians should prescribe no greater quantity than needed for the expected duration of pain severe enough to require opioids.”
Unfortunately, these reports – and the legislation that followed -- created barriers to effective pain relief for many people with chronic pain who previously had good symptom relief with little or no harm from opioids prescribed by experienced clinicians. In the hospice context, the risk of OUD-related harm is exceedingly low when seriously ill patients with moderate to severe pain are managed by appropriately trained medical staff. This is not because expected death renders the development of OUD irrelevant, but because -- at least in my experience with thousands of patients -- OUD does not occur when pain and shortness of breath are appropriately managed with opioids. This includes many patients who were treated for and cured of serious illness or painful orthopedic conditions who successfully stopped taking appropriately prescribed opioids without developing OUD.
In short, OUD is not a concern for hospice patients – and it should be noted that both CDC guidelines specifically exclude patients at the end of life from their recommendations.
Opioids fall into three distinct chemical categories, those related to morphine, such as codeine, oxymorphone (Opana), oxycodone (including OxyContin), buprenorphine (various brand names, including Suboxone), hydromorphone (Dilaudid), and hydrocodone (Vicodin, Lortab), those related to fentanyl, and those related to methadone.
Practically, the opioids are divided by duration of action and potency. Most, including those commonly used in hospice, such as morphine and hydromorphone, provide relief of pain and shortness of breath for about 4 hours. Some of these come in longer-acting oral formulations, such as MSContin and OxyContin, which last 6 to 8 hours and only exist in oral form (remember that long-acting pills will lose their 6 – 8 hour duration of action if they are crushed). Morphine and hydromorphone also come in oral concentrates, which need only be taken under the tongue to work (making them effective for people who have difficulty swallowing), and injected forms. Typically, oral opioids (swallowed or under the tongue) take about 30 to 45 minutes to take effect, IV forms work in 5 – 15 minutes, and those given by intramuscular injection or under the skin (“sub-q”) take about 15 – 20 minutes to work. Oxycodone only has an oral form. The potency of opioids is usually contrasted with morphine and referred to as oral morphine milligram equivalent, or MME. Hydromorphone is roughly 4 – 7 times as potent as morphine, and oxycodone about 1.5 times as potent. Injected opioids are more potent than oral opioids – doses of oral opioids are reduced by half to a third when patients are no longer able to take them by mouth and they are given by injection.
At Connecticut Hospice, we generally start with lower opioid doses given on an as-needed basis for patients who have not previously used opioids (“opioid-naïve”), and we escalate the dose and give it on a scheduled rather than as needed basis as the opioid requirement becomes clear in the first day or two of their use. We always try to schedule these medications to prevent pain or shortness of breath before it starts, rather than relieving it after it has started. Opioid-experienced patients will be escalated as needed from prior dose regimens.
What’s a normal opioid dose? – very variable. Often we start at a dose of morphine 2 mg injected every 4 hours (“Q4H”) in our inpatient unit with the same dose available every 20 minutes as needed (“PRN”) should the scheduled dose be ineffective and an “in-between” dose needed for persistent pain. Hydromorphone 0.4 mg injected Q4H and Q20min PRN is also typical. We then escalate the dose as needed to fully control pain or shortness of breath. While most people need about 5 – 20 mg of injected morphine Q4H or 4 – 8 mg of injected Dilaudid Q4H for effective symptom relief, it is not unusual to get into the thousands of MMEs per day. For this reason, we often say that there is no “ceiling dose” for opioids. (Once, a patient in home care was taking 1300 mg of methadone a day for pain. She was wide awake and able to get around without sleepiness and without pain. Her only complaint was the need to take 130 ten-milligram tablets of methadone every day. By way of comparison, the dose of methadone typically used for the treatment of OUD ranges from about 50 to 150 mg daily.)
Opioid dose is adjusted based on several factors. First, does the dose relieve all the pain? If not, it needs to be increased. Second, does the pain relief last until the next dose? If not, we may need to either increase the dose or decrease the dose interval (e.g., from every 4 to every 3 hours).
How do we choose which opioid to use? Often, this depends on our pharmacy supply. Sometimes, one opioid is preferred over another, depending on a patient’s medical problem. For example, morphine is generally avoided in patients with kidney failure because it can accumulate with a resulting increased likelihood of toxicity or side effects.

Fentanyl is also commonly used in hospice. Fentanyl, which comes in a patch or “transdermal” form that is applied to the skin and replaced every three days, can be very convenient. People need a bit of body fat under the skin for it to work properly, and the medicine will not last 3 days in very underweight people with no fat under the skin.
Methadone is also a very effective opioid. Generally, it is reserved for use in patients still experiencing pain on high doses of short-acting medications such as hydromorphone and morphine. Methadone helps reverse the development of tolerance to other opioids, helping them work in patients who may have been using opioids for a prolonged period and are experiencing reduced effectiveness despite increasing dose – “tolerance.” Methadone can also help people with the painful numbness in the hands and feet – “neuropathy”-- that can affect many patients on chemo- and immune-therapy.
All opioids have side effects – though not the problems with respiratory depression and addiction often ascribed to them, as reviewed above. ALL opioids cause constipation, and patients who are not taking preventive laxatives such as senna or docusate will develop constipation that can be severe and difficult and uncomfortable to overcome. (In fact, most anti-diarrhea medications are weak opioids.) All opioids also cause sleepiness, though the effect usually wears off after a week to 10 days. In hospice, opioid-induced somnolence can be very distressing to families who want to engage with an awake and lucid loved one who is at the end of life, and finding a balance between sedation and pain control can be tricky. For some, a dose of oral methylphenidate, a mild stimulant best known as Ritalin, used for attention deficit disorder, taken in the morning and early afternoon, can help maintain wakefulness while still offering effective pain relief and allowing a night of sleep. Opioids may also cause nausea and a cloudy sensorium. While meds exist to counter these effects, such as haloperidol for nausea, rotating the opioid from, say, morphine to hydromorphone, is often all that is necessary.
Finally, there is the phenomenon of opioid-induced hyperalgesia – a rare condition in which the opioid increases pain sensitivity, resulting in sometimes severe pain from both painful and non-painful stimuli – such as simply being gently touched. This tends to be seen in patients whose pain does not get better – and seems to be getting worse – despite escalating opioid dose, sometime to very high levels. Once hyperalgesia is diagnosed and opioid dose reduced, pain often goes away.
Adjuvants are medications used to help opioids work. A benzodiazepine such as Ativan, for example, used in conjunction with an opioid in a patient with anxiety, can make the opioid more effective. NSAIDS, such as the over-the-counter analgesics ibuprofen and naproxen, have an anti-inflammatory effect and help opioids work. NSAIDS must be used with caution however, as they can cause gastrointestinal bleeding and kidney failure (typically, NSAIDs used for more than a few days are given with an antacid like omeprazole). The literature cites upwards of 16,000 deaths annually due to NSAID-induced gastrointestinal bleeding. Corticosteroid medications such as prednisone and dexamethasone (Decadron) are also powerful anti-inflammatory drugs commonly used as adjuvants for opioids, especially in people with cancer and in those with metastases (spread of cancer) to bone, which can be very painful. Like NSAIDS, corticosteroids have toxicities, including GI bleeding, and are usually used with antacids.
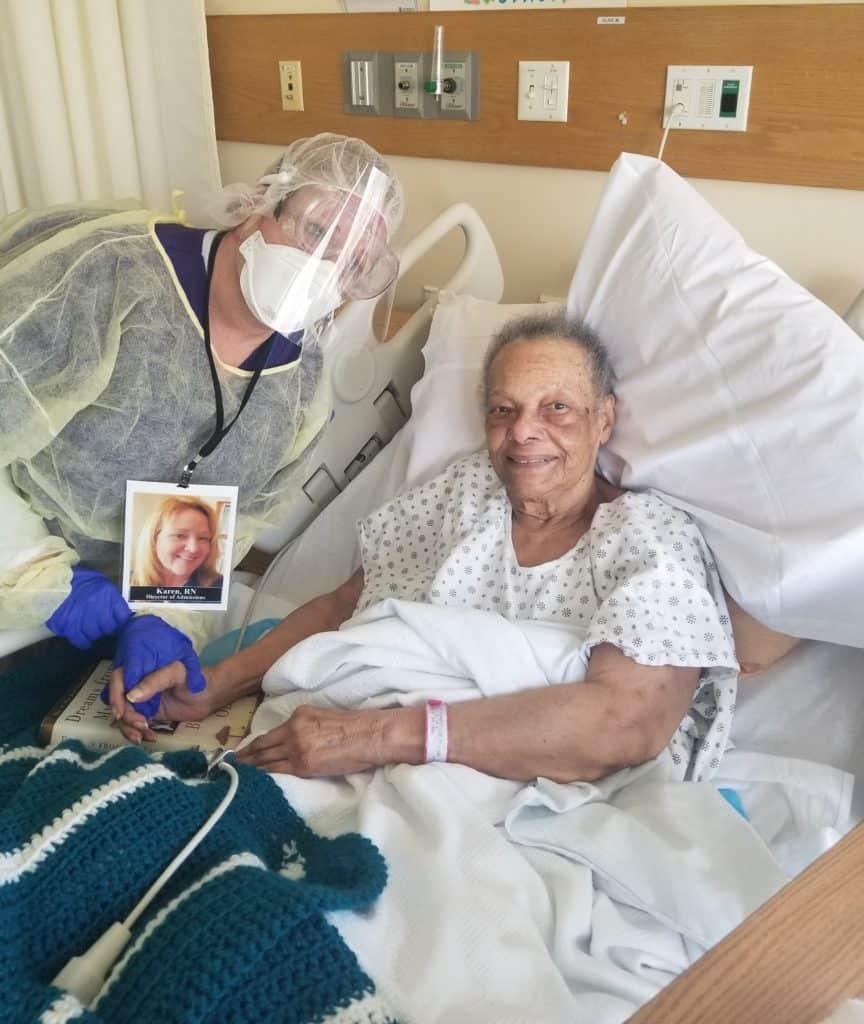
Caring for patients in a hospice setting is a nurturing and supportive effort that draws on the expertise of professionals engaged in many disciplines, ranging from medical to therapeutic. Indeed, the services offered by a leading hospice, such as The Connecticut Hospice, may in fact be broader and the care offered patients more varied than what is typically pictured by members of the public.
Even so, hospice-service providers remain concerned about the number of persons accessing hospice care late in the course of an illness. That’s per a new report issued by the National Hospice and Palliative Care Organization (NHPCO), which states that “53.8 percent of Medicare beneficiaries received hospice care for 30 days or less in 2018.”
More telling, is that fully a quarter (27.9 percent) of the beneficiaries received care for seven days or less— which NHPCO considers “too short a period for patients to fully benefit from the person-centered care available from hospice [providers].”
“This annual report provides a valuable snapshot of hospice care access and care, and also a reminder that we must continue to strive to make hospice care more equitable and accessible,” said Edo Banach, NHPCO president and CEO, in a statement. “It is also important to remember that behind these numbers are people who rely on person- and family-centered, interdisciplinary care to help them during a time of great need.”
Of compelling interest to hospice patients and their family members and friends are sections within the full 26-page report on what hospice care entails, how and where that care is delivered to patients, and what are the levels of care provided.
“Hospice focuses on caring, not curing,” NHPCO observes. “Considered the model for quality compassionate care for people facing a life-limiting illness, hospice provides expert medical care, pain management, and emotional and spiritual support expressly tailored to the patient’s needs and wishes. Support is provided to the patient’s family as well.”
The report also points out that, in most cases, “care is provided in the patient’s home but may also be provided in freestanding hospice facilities, hospitals, and nursing homes and other long-term care facilities. Hospice services are available to patients with any terminal illness or of any age, religion, or race.”
Indeed, the term “hospice” is somewhat elastic. It describes any approved provider of hospice services, including those that operate free-standing hospice inpatient hospitals and those that bring hospice care directly to patients where they are, be that a long-term care facility or in their own home.
The Connecticut Hospice (also known as CT Hospice) fits both descriptions, as it operates its own hospice hospital in Branford and fields teams of hospice medical professionals and caregivers to provide services at other caregiving facilities where patients are residing or right in the patients’ homes.
When hospice services are provided as in home, a family member typically serves as the primary caregiver and, when appropriate, helps make decisions for the terminally ill individual, notes NHPCO. “Members of the hospice staff make regular visits to assess the patient and provide additional care or other services. Hospice staff is on-call 24 hours a day, seven days a week. The hospice team develops a care plan that meets each patient’s individual needs for pain management and symptom control.”
An interdisciplinary hospice team usually consists of the patient’s personal physician, hospice physician, nurses, hospice aides, social workers, bereavement counselors, clergy or other spiritual counselors, trained volunteers, and speech, physical, and occupational therapists, if needed.
NHPCO lists these as interdisciplinary team services:
Nancy Peer, an Associate Professor for Hospice and Palliative Care at Central Connecticut State University, secured a bed for her son, Brian, who was dying of testicular cancer, so he could live out his last weeks at CT Hospice. “Every nurse that came in was not only compassionate… they would see how our son was doing and then they wanted to know how they could help us,” Peer recently told the Daily Nutmeg of New Haven.
Peer said that during the week Brian spent at the hospice, before dying at age 39 and leaving behind his wife of one year and his parents and a younger brother, friends and extended family were able to visit him and Peer and her daughter-in-law stayed with him. She remarked that the help he and his family received from CT Hospice was “priceless.”
The NHPCO report also details the four Levels of Care (as defined by the Medicare hospice benefit) that hospice patients may require. The levels are distinguished by the intensities of care provided relative to the course of a given patient’s disease.
“While hospice patients may be admitted at any level of care, changes in their status may require a change in their level of care,” NHPCO explains. “The Medicare Hospice Benefit affords patients four levels of care to meet their clinical needs: Routine Home Care, General Inpatient Care, Continuous Home Care, and Inpatient Respite Care.”
The report rightly credits the significant positive impact of hospice-care volunteers. “The U.S. hospice movement was founded by volunteers” and they “continues to play an important and valuable role in hospice care and operations.”
But volunteering is not a simple matter of stepping up to help others. The Connecticut Hospital, for example, requires that prospective volunteers receive a background check before coming onboard and then they are professionally trained by hospice staff to provide care and assistance to patients and their loved ones.
The importance of volunteers is underscored by NHPCO’s observation that “hospice is unique in that it is the only provider with Medicare Conditions of Participation requiring volunteers to provide at least 5% of total patient care hours.”
Volunteers typically provide service to others in these three general areas:

Spending time with patients and families (“direct support”)
Providing clerical and other services that support patient care and clinical services (“clinical support”)
Engaging in activities such as fundraising, outreach and education or serving on a board of directors (“general support”)
For information on volunteer opportunities with The Connecticut Hospice, please go to our website, www.hospice.com, or contact Joan Cullen at [email protected] or 203-315-7510.
The Connecticut Hospice is America's first hospice. It was founded by Florence Wald, and a group of nurses, doctors, and clergy, in 1974 and was the first of its kind in the United States. A few years prior, Wald, then an Associate Professor and Dean of the Mental Health and Psychiatric Nursing Program at Yale University, was inspired by a palliative care lecture given by Dr. Cicely Saunders, the founder of St. Christopher’s Hospice, the first hospice in the world.
Today, CT Hospice’s services encompass both in-home and inpatient care for persons diagnosed with a terminal illness with a limited prognosis, normally of six months or less.
The Connecticut Hospice’s central commitment is to enable the patient to live as fully and completely as possible during the time of their illness. This includes supporting the entire family as the unit of care, rather than just the patient. For example, home-care programs are designed to make it possible for families to keep the patient at home if such care is appropriate, and to marshal community resources to help deepen support and keep care costs as low as possible.

We are delighted that clinical rotations have recommenced at Connecticut Hospice, following a temporary hold forced by COVID-19.
On July 13 CEO Barbara Pearce and Medical Director Dr. Joseph Sacco welcomed Hospice and Palliative Care Fellows Dr. Alex Choi and Dr. Bryan Terry for orientation prior to their rotations with Connecticut Hospice in partnership with Yale-New Haven Medical Center's Hospice and Palliative Medicine Fellowship Program.
While at Connecticut Hospice, they will spend time Inpatient and in Home Care with the Interdisciplinary Team, and will expand their knowledge and experience in all aspects of hospice and palliative care, including:
Recognized nationally and internationally as a pioneering hospice and palliative care teaching institution through its educational branch, The John D. Thompson Hospice Institute for Education and Learning, Connecticut Hospice is proud to share its expertise with clinicians from around the country and the world. We look forward to welcoming Dr. Faisal Radwi of Saudi Arabia shortly.

On June 24, Connecticut Hospice welcomed Dr. Nathan Wood, a Yale Primary Care Internal Medicine Resident, to a 2-week rotation with our Medical Department and the Interdisciplinary Team. Connecticut Hospice’s care-providers are not only proud to share their hospice and palliative care experience with new healthcare practitioners, but also pleased to receive additional knowledge from visiting practitioners.
Dr. Wood has published on a variety of topics, including hands-on curriculum for teaching practical nutrition, code-switching in medical settings, and the effects of fibromyalgia on long-term analgesic outcomes following total knee and hip replacement surgery.
Dr. Wood is also a graduate of the Institute of Culinary Education, where he won the Top Toque Award, presented by faculty for highest academic achievement. In 2017 and 2018 he worked as a Medical Student Producer for the Dr. Oz Show, and won a Production Award from The National Academy of Television Arts and Sciences Daytime Emmy Awards. Obviously a man of many talents, our patients and staff have had the pleasure of hearing him play classical piano in our inpatient lobby when not practicing bedside medicine.
This is the first medical rotation since COVID-19 forced a temporary hold on clinical rotations at Connecticut Hospice. All rotations now include orientation on the correct use of PPE (Personal Protective Equipment) during the coronavirus pandemic.
In July three additional Hospice and Palliative Care Fellows will arrive for orientation prior to each performing a one-month rotation Inpatient and an additional two weeks in Home Care with our teams. We look forward to welcoming Dr. Faisal Radwi, Dr. Alex Choi, and Dr. Bryan Terry.
The John D. Thompson Hospice Institute for Education, Training and Research, Inc. (JDT), the educational ally of Connecticut Hospice, was established in 1979 to provide a vehicle for sharing hospice and palliative care philosophy, experience and skills with students, health care professionals, administrators, caregivers, and the community.
The JDT Hospice Institute offers high-quality continuing education services to physicians and nurses and is accredited to award both CMEs (Continuing Medical Education) and CNEs (Continuing Nursing Education). The Institute is also a premier clinical rotation site and annually host over 300 students from prestigious universities located both in and out of Connecticut and around the world.
To learn more, click here: The John D. Thompson Hospice Institute for Education, Training and Research
As a not-for-profit, we depend on generous donors to help us provide customized services and therapies that aren’t completely covered by Medicaid, Medicare, or private insurance.
Please make a gift to help us sustain the highest standard of care.
Admissions may be scheduled seven days a week.
Call our Centralized Intake Department: (203) 315-7540.