A Guide to Hospice Bereavement Support for Families
When someone you love passes away, the support you need doesn’t end with the last day of care. Bereavement support in hospice care is designed to accompany families through the days and months that follow, offering structure, connection, and compassion during the first year of grief (and beyond).
At The Connecticut Hospice, bereavement support is not an add-on service; it’s a core part of how we care for patients and the people who love them. Read on to learn more about hospice bereavement support, including what it involves and how it supports those who have experienced loss emotionally, socially, and spiritually.
Important Takeaways
- Bereavement support in hospice care is a Medicare benefit, offering families structured grief support for at least 13 months after a loved one’s death.
- Hospice bereavement support includes individual outreach, referrals, and hospice grief support groups.
- Through an interdisciplinary team approach, support begins before a loss and continues with coordinated, compassionate care for families.

Bereavement Support Is a Hospice Medicare Benefit
Many people understand that hospice care provides nursing, aides, medications, medical equipment, and 24/7 support. However, fewer realize that bereavement support in hospice care is also included under the Medicare hospice benefit.
Hospice programs are required to offer grief support to family members for at least 13 months following a patient’s death. That timeline exists for a reason: grief rarely moves in a straight line, and important milestones, holidays, and anniversaries often bring renewed emotion long after the funeral.
In healthcare, it is unusual for services to extend so intentionally to surviving loved ones. But in hospice, it’s expected.
When Bereavement Support Begins
At The Connecticut Hospice, bereavement support begins at admission. Our social workers conduct an initial evaluation, including a bereavement risk assessment.
Some families enter hospice already navigating anticipatory grief (the emotional process that begins before a loss occurs). Others may have complicating factors, such as limited support systems, prior trauma, or intense caregiving strain. Our clinicians use their experience and clinical training to identify who may need additional support, both during care and after.
Spiritual care counselors and members of the interdisciplinary team collaborate closely. Hospice care addresses the whole family unit, not just the patient, and that includes emotional and spiritual well-being.
How Hospice Bereavement Supports Loved Ones
Grief affects every aspect of life, from daily routines to long-term well-being. For this reason, hospice bereavement support addresses both practical and emotional needs. This may look like:
- One-on-one conversations with a bereavement counselor to process your loss in a safe, compassionate space
- Practical and emotional support as you navigate the challenges that accompany grief, whether that’s managing daily tasks or working through complex feelings
- Referrals to therapists or psychiatrists when more intensive mental health care would be beneficial
- Grief support groups tailored to specific experiences or identities—for spouses, parents, children, or anyone seeking connection with others who understand
Some people benefit most from individual counseling. Others find solace in group settings where shared stories create understanding. Many use a combination of both. We work with you to identify what feels most supportive at each stage of your journey.
The Role of the Interdisciplinary Team
Hospice care is delivered by an interdisciplinary team comprised of nurses, aides, physicians, social workers, chaplains, therapists, and other specialists who meet regularly to review each patient’s and family’s needs.
Grief, stress, and family dynamics are part of those discussions. If a nurse notices exhaustion in a spouse or an aide observes emotional withdrawal in an adult child, that information is shared, and support is coordinated. This collaborative approach ensures that hospice bereavement support is thoughtful and proactive, rather than reactive.
Members of the team may provide support in different ways:
- Nurses and physicians offer guidance about what to expect physically at the end of life, helping families feel prepared
- Hospice aides provide steady presence and notice subtle changes in mood or coping during day-to-day care
- Social workers facilitate family conversations, address anticipatory grief, and connect loved ones with counseling or community resources
- Chaplains or spiritual care counselors support individuals of any faith, tradition, or belief system as they wrestle with meaning, legacy, or unresolved questions
- Expressive arts therapists and specialists create space for memory-making, reflection, and emotional expression
No single person carries the full weight of support. The strength of hospice bereavement support lies in how those perspectives come together around each family as a cohesive unit.
Continued Follow-Up From the Hospice Team
In the immediate days following a death, many people describe feeling numb. Exhaustion from weeks or months of caregiving often sets in. Practical responsibilities can feel overwhelming or even impossible.
Members of the care team reach out to express condolences. The Bereavement team then begins ongoing follow-up through phone calls, letters, and other touchpoints over the months ahead.
It is common for families not to remember those early calls. That is why contact continues at later intervals. Grief changes over time, and support may feel more accessible weeks or months after a loss than it does in the first few days.
Hospice Grief Support Groups
Grief can feel isolating, even when friends and family are present. Many people find comfort in support groups, which offer the opportunity to meet with others who are navigating a similar loss.
Most grief support groups meet over several months, allowing trust to build gradually. Conversations often shift with the seasons: preparing for the first holiday, navigating anniversaries, or adjusting to new routines and roles. Many participants continue informal connections long after the structured group ends.
Families often share that there is something uniquely reassuring about speaking with others who understand the bereavement experience firsthand. As one participant shared with us, her friends and family had been supportive, but it was invaluable to be in conversation with others who had gone through the death of a parent, just as she had.
Grief Support Groups at The Connecticut Hospice
The Connecticut Hospice currently holds the following bereavement support groups:
- A drop-in General Grief Support Group at our Branford facility
- Eight-week closed support groups in spring and fall, including specialized groups such as Loss of Spouse or Loss of Parent
Importantly, our hospice grief support groups are open to all members of the broader community, not just to families we have served.
The Connecticut Hospice offers hospice grief support groups for spouses, parents, adult children, and other loved ones. Some groups are structured around shared relationships or life experiences, while others are unique to identity, creating space for common concerns that can feel easier to explore among peers.
For example, in 2025, The Connecticut Hospice partnered with New Haven’s Rainbow Elders and Friends to create an online LGBTQ+ grief support group. This collaboration helps ensure that members of the LGBTQ+ community have access to affirming, culturally responsive bereavement support in hospice care. Grief can be shaped by family structure, chosen family, identity, and past experiences with healthcare systems, and having this dedicated space for support and healing matters.
If you would like to participate in a support group, please contact our Bereavement Department at (203) 315-7455 or email bereavement@hospice.com.

Supporting Families—and the Professionals Who Care for Them
Hospice professionals encounter grief every day. They are trained to recognize how loss can surface: sometimes as sadness; sometimes as anger, withdrawal, or frustration. Maintaining compassion in those moments requires both emotional presence and professional resilience.
The Connecticut Hospice social workers play an important role in these experiences. They help clinical staff process difficult interactions, navigate intense family dynamics, and respond thoughtfully rather than reactively. That internal support strengthens the care families experience. When caregivers feel supported, they are better able to remain steady and patient during emotionally charged moments.
When Grief Evolves Into Service
Some individuals find meaning in staying connected to hospice after their year of bereavement support. Many of our most dedicated volunteers once sat in a grief support group themselves.
We encourage families to allow time—typically a year—before volunteering. Early grief needs space. But when the time is right, supporting others as a hospice volunteer can be a powerful way to honor a loved one and continue their legacy.
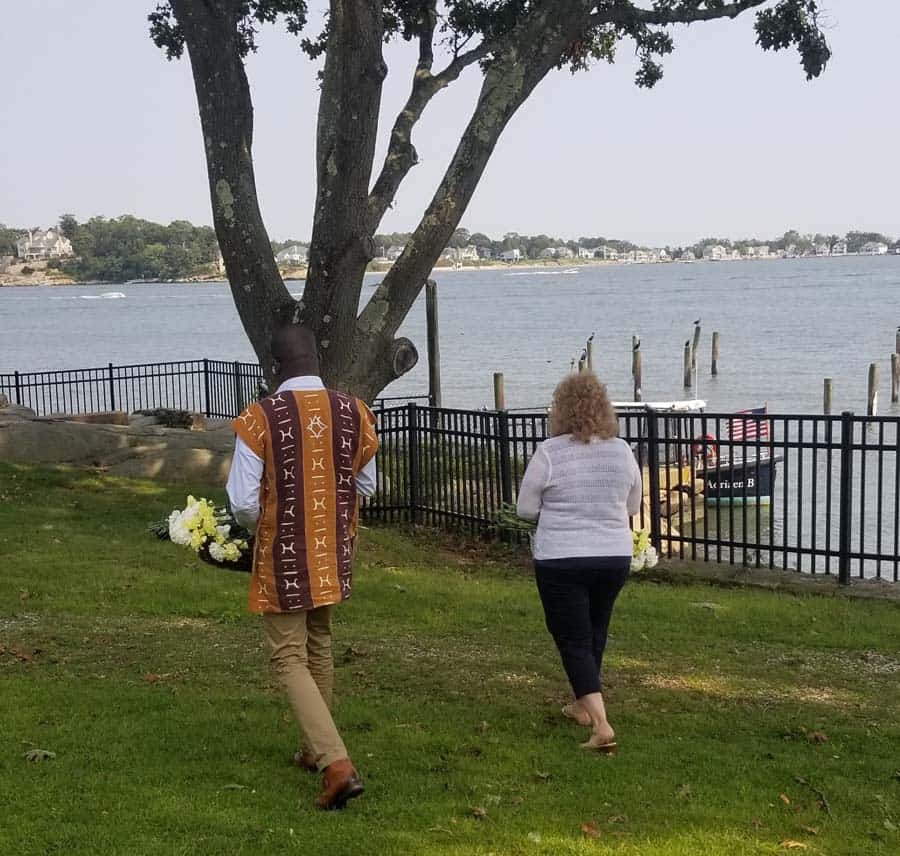
The Connecticut Hospice’s Annual Ceremony of Remembrance
Each year, The Connecticut Hospice holds a Ceremony of Remembrance honoring our patients who have passed in the prior year. While separate from our ongoing bereavement services, the ceremony is a cherished annual tradition that brings our community together in collective remembrance.
For this ceremony, family, friends, and staff gather at our Branford facility (or join online via live stream) to reflect and honor loved ones, each of whom is recognized by name and photograph. At the end of the service, music fills the air, while flowers representing those who have passed are carried in baskets down to a boat on the shore. The boat slowly makes its way out to the water, and the flowers are gently released, floating as a beautiful tribute to lives well-lived. The ceremony is even timed with the tides, honoring the natural rhythms of the shore.
These rituals acknowledge that every life leaves an imprint and that grief deserves sacred space. In remembering together, we find comfort, connection, and meaning.

Support Through the Days That Follow
Bereavement support in hospice care exists because loss reshapes daily life, identity, and relationships. Support may take the form of a phone call, a group conversation, a written resource, or simply the knowledge that someone will check in again.
At The Connecticut Hospice, we consider it a privilege to walk alongside families—not only for patients at the end of life, but for their loved ones in the months and years that follow. We remain available with guidance, resources, and support whenever needed.
Grief can feel isolating, but you don’t have to carry it alone. If you or someone you love could benefit from bereavement support, we invite you to reach out today. We’re here to listen.






